Why Falls Are the Silent Epidemic in Indian Elderly Care
Falls are the leading cause of injury-related death in people over 65. In India, with 194 million elderly and almost no trained fall-prevention specialists, the scale of the problem is staggering.
Falls in the elderly are not accidents — they are predictable, preventable events that represent a failure of the healthcare system to intervene early. In India, where senior healthcare infrastructure is almost nonexistent, falls represent one of the most urgent and underaddressed public health crises.
The Scale of the Problem
Globally, falls are the second leading cause of accidental injury deaths, after road traffic accidents. In people over 65, they are the leading cause. One in three adults over 65 falls each year; one in two over 80. Of those who fall, 20–30% suffer moderate to severe injuries — fractures, head trauma, lacerations — that reduce mobility and independence.
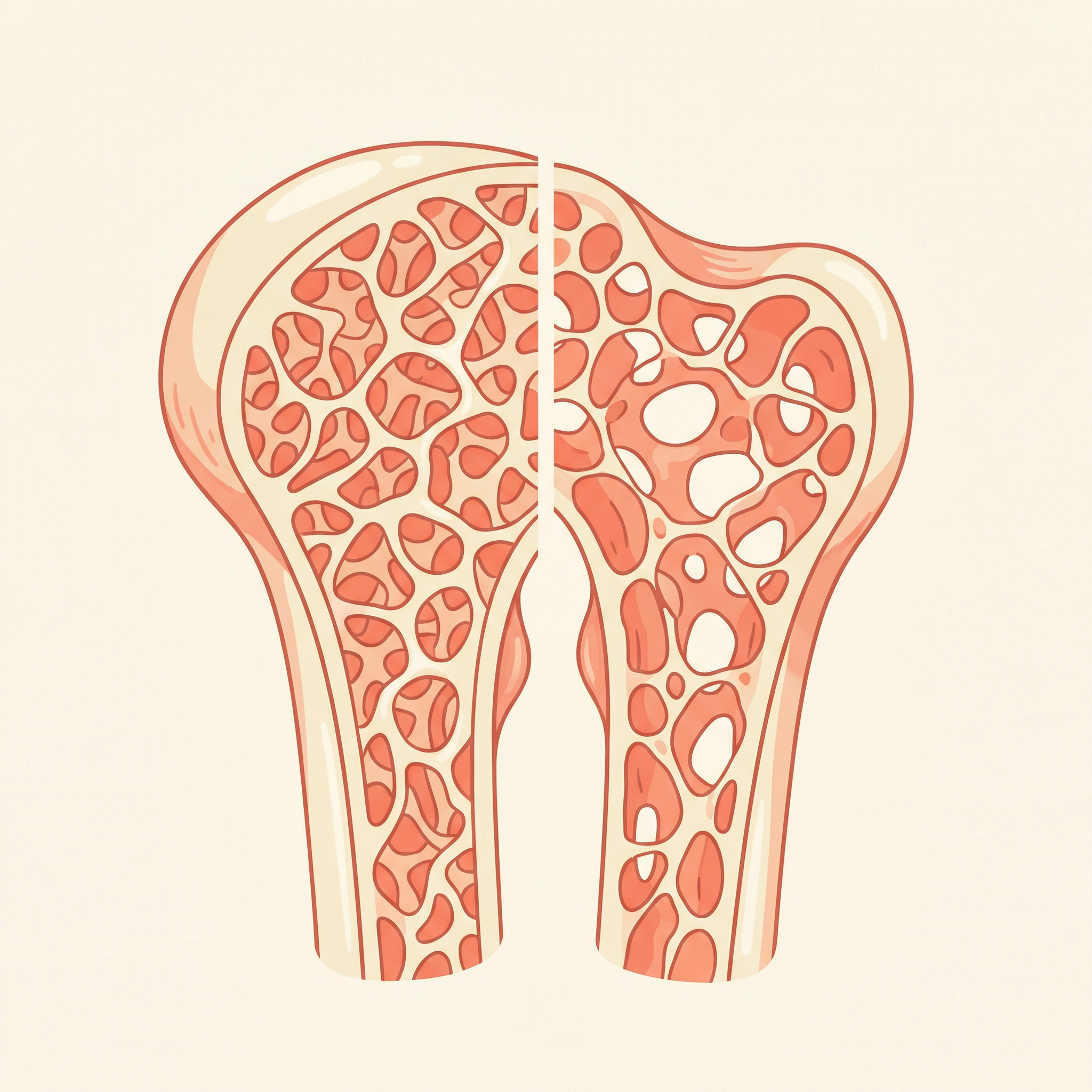
In India, with 194 million elderly citizens and a healthcare system primarily oriented toward acute disease, the burden is enormous. Hip fractures alone — the most serious consequence of falls — carry a one-year mortality rate of 20–30% in elderly patients, and survivors often never regain their pre-fracture level of function.
Why Falls Happen: The Multifactorial Model
Falls are not caused by a single factor — they are the result of multiple interacting risk factors that accumulate with age:
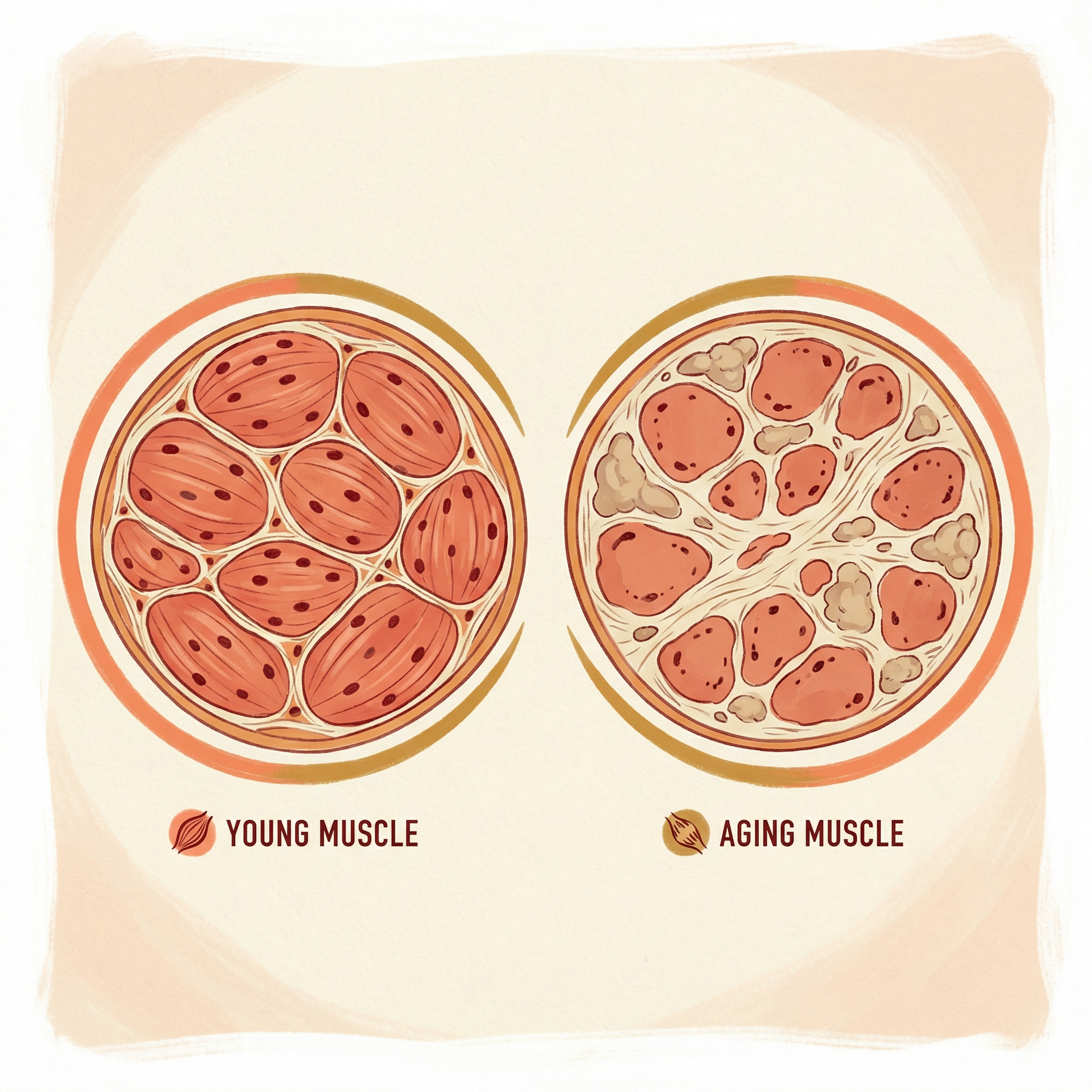
- •Muscle weakness: Sarcopenia reduces the strength needed to recover from a stumble
- •Balance impairment: Vestibular function, proprioception, and visual acuity all decline with age
- •Gait changes: Slower gait speed, reduced stride length, and increased double-support time
- •Medication effects: Sedatives, antihypertensives, and diuretics increase fall risk
- •Environmental hazards: Uneven floors, poor lighting, loose rugs — common in Indian homes
- •Cognitive impairment: Reduced attention to environmental hazards
- •Orthostatic hypotension: Blood pressure drop on standing, causing dizziness
The Tinetti Fall Risk Assessment and the STEADI (Stopping Elderly Accidents, Deaths, and Injuries) toolkit are validated instruments for identifying high-risk individuals — tools that PHA coaches are trained to use.
The Fear of Falling: A Secondary Problem
After a fall, many elderly individuals develop a fear of falling that leads them to restrict their activities. This restriction — while understandable — accelerates the very deconditioning that increases fall risk. The fear of falling becomes a self-fulfilling prophecy.
Breaking this cycle requires building genuine confidence through supervised exercise. When an elderly patient successfully completes a challenging balance exercise in a safe environment, with a trained coach present, their confidence grows alongside their physical capacity.
Evidence-Based Fall Prevention
The evidence for exercise-based fall prevention is among the strongest in all of geriatric medicine. A 2019 Cochrane review of 108 randomised controlled trials found that exercise reduces falls by 23% and fall-related injuries by 27% in community-dwelling older adults. The most effective programs combine:
- •Balance training (single-leg stands, tandem walking, perturbation training)
- •Strength training (lower limb focus — quadriceps, hip abductors, ankle dorsiflexors)
- •Functional training (sit-to-stand, step-ups, reaching tasks)
What Praan Health Coaches Do
PHA coaches conduct formal fall risk assessments using validated tools, design individualised fall prevention programs, educate patients and families on environmental modifications, and coordinate with physicians when medication review is indicated. This comprehensive approach — addressing both the physical and environmental determinants of falls — is what distinguishes a trained senior healthcare specialist from a generic fitness trainer.
References & Further Reading
- [1]Peel NM. Epidemiology of falls in older age. Can J Aging. 2011;30(1):7-19.
- [2]Sherrington C et al. Exercise for preventing falls in older people living in the community. Cochrane Database Syst Rev. 2019.
- [3]Tinetti ME, Williams CS. Falls, injuries due to falls, and the risk of admission to a nursing home. N Engl J Med. 1997;337(18):1279-84.
Category
Learn This in 21 Days
Everything in this article is taught in depth during the PHA certification program.
Enroll FreeReady to Apply This Knowledge?
The PHA 21-day certification teaches you to apply evidence-based senior healthcare with real patients.